
Pregnant women in the United States are increasingly experiencing adverse maternal and birth outcomes. The maternal mortality rate in 2019 was 20.1 deaths per 100,000 live births, which is an increase from 17.4 in the previous year.1 For Black, Indigenous, and people of color (BIPOC), the rates were 2.5 and 3.5 times higher, respectively, compared with non-Hispanic White women.2 The rate of preterm births also continues to rise, particularly among BIPOC populations, and overall one in ten infants is born preterm.3 Infants born preterm or with low birthweight are at an increased risk for experiencing physical disabilities and developmental impairments throughout their lives.
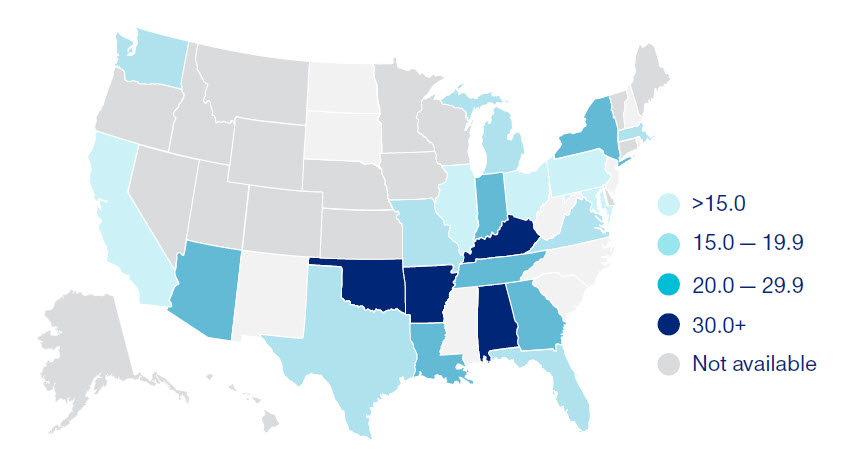
Number of deaths per 100,000 births4
With approximately half of all births in the United States covered by Medicaid, Medicaid managed care organizations and their state partners have the ability to improve health outcomes among Medicaid consumers.5 Together, we can develop prenatal care management and postpartum coverage strategies to support healthy pregnancies and birth outcomes. We are also both uniquely positioned to address the disparities and health inequities that exist for pregnant and parenting individuals accessing Medicaid.
20
The U.S. maternal mortality rate is rising, with 20 deaths for every 100,000 live births.1
8%
Low birthweight impacts 8% of all infants born.3
1/2
1/2 of all births in the U.S. are covered by Medicaid.5
Key Medicaid maternal health policy and program design features
Focus on disparities and inequities. Emphasize action to address the disparities that exist for pregnant individuals accessing Medicaid, particularly BIPOC. This includes supporting strategies focused on addressing the racial, ethnic and geographic disparities in maternal health outcomes.
Ensure access to care. Streamline eligibility to ensure that needed services and supports are received early in the prenatal stage of pregnancy. Additionally, coverage should continue up to one-year postpartum to positively impact health outcomes for both parenting individuals and babies.
Provide comprehensive benefits. Ensure access to a comprehensive array of benefits to support healthy pregnancy, full-term delivery, and access to critical physical, behavioral, and social services and supports needed postpartum.
Evolve care access modalities. Continue to adopt digital platforms and mobile-friendly strategies to encourage engagement, support education, and allow for virtual support and monitoring of pregnant individuals during the prenatal stage of pregnancy, and for both mom and baby postpartum.
Examples of state maternity solutions in action

Since the 2006 creation of the California Maternal Quality Care Collaborative, which is focused on ending preventable morbidity, mortality and racial disparities in maternal care, California has seen its maternal mortality rate decline by 55% while the rest of the nation has experienced increases.6

Women who are provided access to doulas in Minnesota are 22% less likely to have a premature birth compared with women covered by Medicaid who do not use a doula.7

Through a project of the Tennessee Initiative for Perinatal Quality Care, the state has been able to increase the number of pregnant individuals with opioid use disorder who receive Medication Assisted Treatment from 45% to 72%.8
Sources
- Hoyert D. Maternal Mortality Rates in the United States, 2019. National Center for Health Statistics. Published April 2021. Accessed May 5, 2021.
- March of Dimes. Low birthweight. Published March 2018. Accessed May 5, 2021.
- Ibid.
- Declercq E, Zephyrin L. Maternal Mortality in the United States: A Primer. The Commonwealth Fund. Published December 16, 2020. Accessed May 5, 2021.
- Kaiser Family Foundation. Births Financed by Medicaid. Published 2019. Accessed May 5, 2021.
- California Maternal Quality Care Collaborative. Maternal Mortality Rates, California and United States; 1999-2013. Accessed May 5, 2021.
- Benson L. U study finds doulas improve birth outcomes, cut costs. MPR News. Published January 14, 2016. Accessed May 5, 2021.
- The Impact of the Tennessee Initiative for Perinatal Quality Care. Opioid Use Disorder: Optimizing Obstetric and Neonatal Care Project - Maternal Arm. Accessed May 5, 2021.